If you’re here to learn about primary hyperparathyroidism, caused by a hyperparathyroid adenoma, I understand the fear. The name alone is overwhelming!
I went through all the emotions when I was diagnosed with primary hyperparathyroid disease. My “routine physical” last year, turned out to be anything but!
I’d been eating healthy (healthier, anyway) and exercising regularly. So, when my doctor told me I had high blood pressure, out of control cholesterol and osteoporosis, I was really upset.
She expected primary hyperparathyroidism and sent me to the specialists.
As I went to the endocrinologist and the surgeon, I was frustrated that my body was sabotaging me. I was overwhelmed by emotions as I grappled with how a tiny little gland, the size of a grain of rice, had stolen the calcium from my bones to make me very sick.
I get it. If you’re afraid, overwhelmed and frustrated, I was there. If you find yourself crying a lot, I did too.
But…
Let me reassure you. Primary hyperparathyroidism (or PTH) is a lot harder to spell than it is to treat!
So, let’s get to the nuts and bolts of this thing!
- What is primary hyperparathyroidism?
- What are the symptoms of hyperparathyroidism?
- What will happen at the endocrinologist’s office?
- What can I do to help my body while I wait for surgery?
- What should I expect with parathyroid surgery? (It’s pretty much the only real option.)
- How do I take care of my scar after a parathyroidectomy?
I had all these questions and more! I hope this post reassures you that you can help your body, surgery isn’t all that bad, and you can undo some of the damage that was done by that parathyroid adenoma.
I am not a physician. This post in no way should be used as a substitute for medical care. Ask your doctor if you have questions about your health — those initials after a doctor’s name mean they know a thing or two!
what is primary hyperparathyroidism?
Primary hyperparathyroidism is caused by a parathyroid adenoma — I heard cancer, of course. But, an adenoma is a benign tumor that causes the parathyroid gland to get hyper about doing its job.
The overactive gland doesn’t settle down when it should, sending body chemistry into chaos.
My doctor showed me my lab results for parathyroid hormone levels (PTH) and blood calcium levels. Both were in the normal range, so I was confused.
But, she explained that PTH and calcium work like a teeter-totter.
When one is high, the other should be low. The PTH level rises when the body needs more calcium, signaling the bones to release it into the bloodstream.
When the body has sufficient calcium, the PTH level should drop low.
With primary hyparathyroidism, that doesn’t happen. Both the PTH and calcium levels stay high creating a body chemical mess of too much calcium. Since calcium is important to regulating many things in the body, when it’s not right, we get sick.
What are the symptoms of a parathyroid adenoma?
The symptoms of Primary Hyperparathyroidism are known as “moans, groans, bones and stones.”
The moans and groans comprise a number of symptoms:
- Fatigue,
- Body aches,
- Muscle aches,
- Sleeplessness,
- Grumpiness (unexpectedly snapping at family members especially),
- Depression,
- Brain fog.
These are common symptoms. I had all of them — but I attributed them to other things in my life.
- I had been exercising for the past year, going to the gym 3-5 times a week. I thought the muscle aches, body aches and fatigue were related to trying to get healthy in midlife.
- My husband went through an unexpected job change. Two weeks after starting his new job, one of our bathrooms flooded overnight causing more than $40,000 damage to our home. I thought the sleeplessness, grumpiness and “depression” were caused by the stress.
- To be honest, the brain fog was a bit scary. I couldn’t come up with words sometimes. I couldn’t remember short lists when I went to the store. Sitting at the dinner table, I’d struggle to find words to keep up with simple conversation. More than once, I was afraid I might be developing Alzheimer’s.
Parathyroid tumor symptoms are vague and increase as the condition gets worse.
The subtle changes happen over time, so people don’t generally recognize a health issue.
Like me.
I went to the doctor specifically for complaints of muscle and leg aches in 2011 and 2015. My doctor ran the tests, but didn’t notice that — while in the normal range — my PTH and calcium were elevated. He attributed it to needing more exercise, more sleep and better diet. He ordered bone density scans both times, noting that I had osteopenia and needed to exercise more.
He missed the root cause. Lots of doctors do, but I am still mad about it.
Besides the physical symptoms listed above, primary hyperparathyroidism can cause kidney stones and osteopenia (or osteoporosis if not caught until late). Osteopenia is a thinning of the bones, indicating insufficient calcium.
My new doctor ordered a bone density scan to see if my osteopenia had worsened. Unfortunately, mine had progressed to full osteoporosis in my spine and worsened osteopenia in my hips.
The emotional “side effects” of hyperparathyroidism
Our daughter is seven years younger than her next older sibling. When her brother left for college, I was determined to make sure it was a special time for her. She’d had to follow big brothers around all her life. It was finally her turn to be the center of attention.
But, the fatigue, frustration, depression and exhaustion of primary hyperparathyroidism made that very difficult.
For instance, I’d decide to make Valentine’s Day cookies to put in her lunch as a surprise. But, after she’d go to bed, I couldn’t. I had nothing in me.
Or, before school, she would ask if we could play a board game after school. I’d say yes, but by the time she got home, I’d be so tired, I just couldn’t.
I wondered if I didn’t love her like I should. I wonder if she thought I didn’t love her as much as her brothers.
It wasn’t just her. I had very little energy or patience for my husband, too. There were many tearful nights, and I thought I was losing my mind and ability to be a good human.
What happens at the endocrinologist?
Medical specialists, like endocrinologists, are essential to the treatment plan for hyperparathyroid disease.
Medical specialists read the reports from primary care physicians, but expect more tests anyway.
An endocrinologist is an expert in medicine related to the adrenal system and hormones. Your endocrinologist will want to look for every possible medical condition to develop a proper plan of care. The doctor will probably also request a urine test to determine how much calcium is leaking into the urine — the more calcium, the greater the risk of kidney stones.
At a second visit after all the tests are run and the results are back, the endocrinologist will have sufficient information to determine a course of action.
For most people, the best treatment for primary hyperparathyroidism is surgery, called a parathyroidectomy or parathyroid surgery. If surgery is recommended, the endocrinologist will order an ultrasound of the parathyroid and make a surgical referral.
what can i do to help my body while I wait for surgery?
I’m not one to sit around and wait for things to happen. So, when I got my diagnosis, I knew I had to help my body the best I could. My primary care doctor was a great advocate for self-care. She supported me as I made healthy choices to help my body fight back against the disease.
It turns out I was already doing a lot to help myself with exercise and healthy eating. But, I got more serious about both aspects.
Because of the osteoporosis, I asked my doctor for a referral to physical therapy to strengthen the core muscles that support the body and to improve my balance. When a person with osteoporosis falls, there’s a bigger risk of bone fractures. Physical therapy was a great way to improve balance and strength.
In my case, my blood pressure was really high (150/120, when 120/80 is normal). My lipids — overall cholesterol, LDL and triglycerides — were really high, which is bad. And my HDL, or “good cholesterol,” was really low, which is also bad.
So, I asked my doctor for a referral to a nutritionist to develop a heart healthy diet to help address these issues. Before I even went to surgery, my blood pressure had improved to 130/90 — not normal, but a whole lot closer!
Just because you have a medical diagnosis that causes all these symptoms doesn’t mean you’re helpless! Ask your doctor what you can do while waiting for surgery to improve your health and take control.
An added bonus, after surgery, you will have a head start toward a really healthy life!
What should I expect with parathyroid surgery?
Parathyroid surgery, called a parathyroidectomy, involves removing the overactive parathyroid gland. Most of the time, only one of the four parathyroid glands develops into an adenoma. Even though the parathyroid adenoma is non-cancerous, the surgeon will send the tissue to pathology to confirm that just to be safe.
The day of your parathyroid surgery
The night before surgery, you’ll have to stop eating and drinking, just like any other surgery. Most of the time, a parathyroidectomy is an outpatient procedure.
After getting checked in for surgery, the nurse will prep you. The anesthesiologist will come in to explain how anesthesia works. Either the surgeon or the nurse will explain possible complications to you like sores from laying in bed during surgery (though my hospital took steps against that), a bit of pain or a sore throat, and some slight bruising where the anesthesia tubing goes in.
The surgery itself involves a very small incision across the front of the neck. My surgeon, who specializes in thyroid and parathyroid disease, follows a natural crease in the neck to make the incision.
Throughout surgery, the surgeon will check PTH and calcium levels in real time. To make that easier, an arterial line is inserted into your arm. During surgery, they draw blood from the arterial line and measure calcium and PTH levels to make sure all the troublesome gland has been removed. If levels don’t come down, the surgeon will know to look for another parathyroid gland before closing up the surgical site.
Once the surgeon is done, the incision is closed using techniques much like plastic surgery. My surgeon then used surgical tape to reinforce the incision and protect it from getting pulled in hopes of minimizing the scar.
I went home just a couple hours after surgery, once I could drink, eat and talk. The doctor went over how to care for the incision and when to call him should I have issues. He explained the importance of taking supplemental calcium during recovery.
I expected a sore throat and trouble eating, but had no issues whatsoever. That part of my parathyroid surgery recovery went very well.
Parathyroid surgery complications
There are some complications to watch out for with parathyroid surgery: hypocalcemia (calcium levels too low), bleeding at the incision, hoarse voice and sore throat are the most common.
However, a “medically insignificant” number of people (meaning very, very few) can also develop an arterial thrombosis — which is a blood clot in the artery where the arterial line was put in for the surgical blood draws.
It’s so insignificant, the anesthesiologist might not even tell you about it (mine did not tell me… she just said I’m really healthy other than the parathyroid gland and surgery would be easy).
You should expect some pain while the artery wall heals, but if it gets worse a few days after surgery, call your surgeon and insist on an appointment immediately. If it gets unbearable, go to the ER.
Of course, I got the super rare arterial clot, called arterial thrombosis. It hurt so much more than the parathyroidectomy! It resolved over time, but it was frustrating that no one warned me to watch for it.
After parathyroid surgery
Just a few days after my parathyroidectomy, I felt so totally different I actually giggled at the dinner table!
I wish I could explain it to you, but the fog was gone. My head just felt better — the cobwebs simply vanished and my head felt so much lighter. It struck me suddenly, and I couldn’t help but laugh. I was goofy and fun-loving again.
I enjoyed being with my daughter!
Most people can return to full activities within about two weeks of surgery, though my recovery was slowed by the blood clot.
When I returned to the gym, I went slow the first couple of days. Within two weeks, I was stronger and more energetic than I had been in the months before surgery. I expected improvements, but they were more significant and more quick than I would have guessed.
No surprise, probably, but I also sleep better than I have in years!
How do I take care of my parathyroid surgery scar?
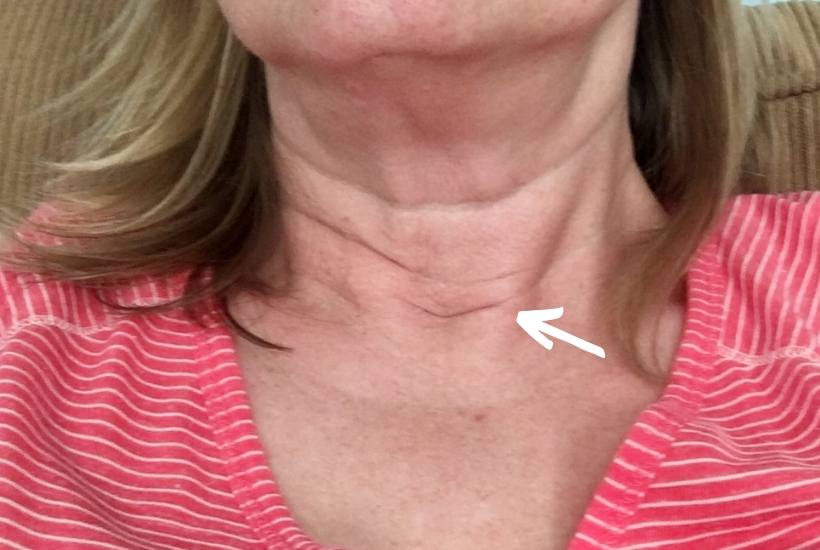
Before surgery, I searched all over the internet for what to expect the scar to look like. I read articles explaining that the scar is small and usually is placed in a neck fold. I couldn’t find much information on how to take care of it or minimize its appearance.
This is my scar, still visible after 5 months. Every few weeks, it’s less visible. Maybe one day, no one will be able to see it.
Here’s how I cared for my parathyroidectomy scar:
- A soft ice pack. When I got home from the hospital, I placed a soft ice pack across my neck for 20 minutes every two hours throughout the day to keep my incision from swelling. This ice pack is great because it’s narrow, not lumpy and comes with 6 inserts so you always have a cold pack ready to go.
- Keep the area clean and don’t pull the skin. Your surgeon will provide specific instructions on how to care for your incision until it closes. Follow those instructions carefully.
- Vitamin E oil. After the wound healed, I gently rubbed Vitamin E oil on my scar three times a day — after my shower, mid-afternoon and before bed. It’s important not to pull the skin, but to massage it in gently. Vitamin E helps minimize scars.
- Sunblock lotion. I use Neutrogena sunblock, SPF 45 for faces, because it’s not greasy. I put this on before leaving the house — every single time! I reapply it throughout the day — even setting reminders on my phone if I’m outside so I don’t forget. The skin in a scar is very delicate and takes more than 6 months to heal. By protecting the scar with a high quality sunblock, I protect that delicate skin. If the scar isn’t protected with sunblock, it will darken in the sun and never fully fade.
That’s really all there is to it. I am hopeful that in the next couple of months, the scar won’t be noticeable at all!
If you’re reading this at 2:00 a.m. because you might (or do) have primary hyperparathyroidism, turn off your screen, close your eyes and rest. This is a very treatable condition.
learn more about hyperparathyroidism (when it’s not 2:00 am)
These professional resources help explain where the parathyroid glands are, how they are supposed to work and what to expect with surgery. Of all the resources out there — some of which are alarmist — these were most helpful to me. I hope they help you.
- Cleveland Clinic — Overview, Diagnosis, Treatment and Prognosis (with images)
- How the Parathyroid Gland is supposed to work — a diagram in almost plain English
- Illustration of the Parathyroid Glands — also includes a detailed list of what to expect after surgery (for information only — follow your doctor’s specific instructions after surgery)



I have just been diagnosed and have spent a lot of the evening crying with worry.
I found your article by default and I’m so glad I did.
After reading it I feel relief and a lot of the fear has diminished,instead I feel calmer and now need to embrace what lies ahead with a positive mindset and knowing my faith is my guidance and strength and god willing,will get me through this.
Thank you so very much .
Dear Karen,
I can’t thank you enough for this post. I was recently diagnosed with hyperparathyroidism. Thankfully my GP followed up on above normal calcium. Your post really describes my feelings and symptoms. It can be overwhelming. I am waiting for surgery and looking forward to getting my health back on track!!! Thanks again